A colleague asked me about Amniotic Membrane and how to place it on the eye.
Ammniotic membrane has multiple factors, such as collagen of various types, laminin, fibronectin, and proteoglycan that promote healing damaged cells. Amniotic membrane has a high tensile strength (its a pretty tough membrane) and induces reepithelialization through chemical mediators. It has multiple anti-inflammatory, antibacterial and antiviral properties acts as a scaffold in which cells can proliferate and differentiate as it has pluripotent cells among its layers. Amniotic membrane does not have any risk of tumor formation according to multiple publications.
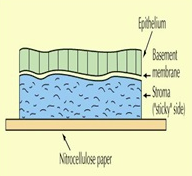
When using amniotic membrane the goal is to face the stromal side towards the cornea and have the epithelial side facing up.
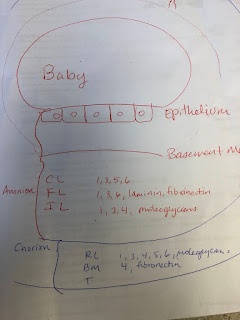
This sketch shows how the baby lies in relation to the exaggerated placental membranes: composed of the Amnion and the Chorion. We use only the amnion as this is a clear membrane with multiple healing factors. The chorion is filled with blood vessels that may not be as desirable in healing the cornea.
References:
References
- Mamede AC, Carvalho MJ, Abrantes AM, Laranjo M, Maia CJ, et al. (2012) Amniotic membrane: from structure and functions to clinical applications. Cell Tissue Res 349: 447–458.
- Insausti CL, Alcaraz A, García-Vizcaíno EM, Mrowiec A, López-Martínez MC, et al. (2010) Amniotic membrane induces epithelialization in massive posttraumatic wounds. Wound Repair Regen 18: 368-77.
- Gruss JS, Jirsch DW (1978) Human amniotic membrane: a versatile wound dressing. Can Med Assoc J 118: 1237-1246.
- King AE, Paltoo A, Kelly RW, Sallenave JM, Bocking AD, et al. (2007) Expression of Natural Antimicrobials by Human Placenta and Fetal Membranes. Placenta 28: 161-169.
- Hartstein B, Gausche-Hill M, Cancio LC (2013) Burn Injuries in Children and the Use of Biological Dressings. PediatrEmerg Care 29: 939-94
Protocol:
https://www.slideshare.net/EBAICME/amniotic-membrane-transplant
References: