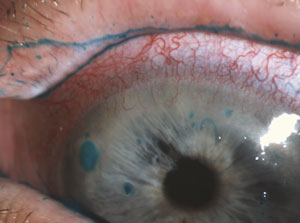
Filamentary Keratitis ICD-9 370.23
Filamentary keratitis is a condition in which strands (“filaments”) composed of degenerated epithelial cells and mucus develop on and adhere to the corneal surface causing pain and foreign body sensation.
The etiology of filamentary keratitis is related to an alteration in the components of the tear film and/or abnormalities of the corneal surface. It is associated with a number of ocular surface diseases and conditions.
Any alteration of the tear film or corneal surface can increase the risk for filamentary keratitis. Common risk factors include: aqueous tear deficiency as in keratoconjunctivitis sicca, corneal exposure (e.g. seventh nerve palsy), occlusion abnormalities such as blepharoptosis, ocular surgery (e.g. keratoplasty), systemic diseases with effects on the ocular surface (e.g. Sjogren’s syndrome), extended use of anticholinergic medications, and other ocular surface abnormalities.
In filamentary keratitis, there is often an increase in the tear film mucus to aqueous ratio. This is commonly due to a decrease in aqueous tear production, but may also be due to increased production or accumulation of the mucinous component. This alteration in tear film makeup sets the stage for formation of mucoid filaments. Small defects in the corneal epithelium provide an anchoring surface for the filaments. Mucin attaches to the epithelial defect and loose epithelial strands are incorporated into the mucin strand attached to the surface. Filaments may be small sessile adhesions or longer strings that cause irritation and discomfort.
It is hypothesized that the initial step in the development of filamentary keratitis is damage to basal epithelial cells, epithelial basement membrane, or Bowman’s layer leading to focal detachments of the epithelial basement membrane. Blinking causes these areas of detachment to become elevated leading to irritation, inflammation, and increased mucus production. The sites of epithelial damage provide the scaffold for filaments to develop. A postmortem analysis of a cornea in a patient with this condition revealed inflammatory cells and fibroblasts just beneath the basal epithelium.
Filamentary keratitis generally occurs in association with an underlying condition. The primary preventative measure is lubrication in the setting of dry eye.
Patients with filamentary keratitis complain of foreign body sensation. They may also have redness, epiphora, blepharospasm, and photophobia.
Slit lamp examination reveals filaments (‘mucoepithelioid” strands) adherent to the corneal surface. The filaments can vary from 0.5mm to 10mm in length. A gray colored subepithelial opacity can sometimes be seen at the base of the filament. Blinking causes painful traction on the filaments and may detach them, leaving behind an epithelial defect. Filaments stain best with rose Bengal, but can be seen with fluorescein as well. The location of the filaments can help determine the underlying cause. Filaments due to dry eye syndromes tend to be found in the interpalpebral space, those due to ptosis superiorly, and those due to surgery at the site of the wound or surgical trauma
Signs include multiple filamentary attachments firmly adherent to the corneal surface, decreased aqueous tears, increased mucin in the precorneal tear film, subepithelial opacities at the base of filaments, or frank corneal epithelial defects.
Symptoms can vary from mild to severe foreign body sensation that is exacerbated by blinking and is associated with photophobia, blepharospasm, and epiphora. The patient may also complain of a red eye.
The diagnosis of filamentary keratitis is made clinically with history and slit lamp biomicroscopy.
Diagnostic procedures[edit source]
Slit lamp biomicroscopy demonstrates firmly adherent filaments on the corneal surface. A Schirmer test may be helpful in establishing the diagnosis of a dry eye syndrome.
There is no specific laboratory testing indicated for filamentary keratitis. However, if suspicion is high for underlying systemic disease that has not yet been diagnosed such as Sjogren’s syndrome, a systemic work-up may be indicated.
Differential diagnosis[edit source]
Corneal filaments are pathognomonic for this condition, but there is a broad differential for the underlying cause of filamentary keratitis. The differential for underlying disease includes tear film abnormalities, lid malpositions, previous ocular surgery, and toxic keratopathies.
The treatment of filamentary keratitis can be challenging and is often chronic. Paramount in the overall treatment of filamentary keratitis is management of underlying conditions such as the dry eye syndromes, medication toxicity, contact lens overuse, and blepharoptosis.
First line treatment includes topical therapy with lubricant drops and ointment. Low water-content bandage contact lenses may be helpful temporarily in cases that do not respond to lubrication alone. The bandage contact lens should be used in combination with artificial tears and prophylactic topical antibiotic. A mucolytic agent such as 10% N-Acetylcysteine can be used topically to decrease the viscosity of the mucinous component of the tear film. Topical sodium chloride drops may also help by deturgescing and compacting the corneal epithelium.
Patients should be re-examined 3-4 weeks after the initiation of medical therapy. Bandage contact lenses should be left in place for no more than one month.
Filaments can be removed at the slit lamp using jeweler’s forceps. Care should be taken to avoid disrupting the epithelium at the base of the filament if possible. Manual removal of the filaments may help in alleviating symptoms temporarily but is only a temporizing measure and is not successful without concurrent medical treatment. Punctal occlusion may also be helpful in cases of underlying aqueous tear deficiency.
Infectious keratitis is a potential complication, especially when a bandage contact lens is used for therapy.
Prognosis depends upon effectiveness in managing the predisposing condition, but is generally good. Patience is often required in the chronic management of this condition.
Davidson RS, Mannis MJ. Filamentary Keratitis. In: Krachmer JH, Mannis MJ, Holland EJ, editors. Cornea. Vol 1. 3rd ed. Philadelphia: Elsevier/Mosby; 2011. P. 1093-96.
Van Meter WS, Katz D, Cook BG. Filamentary Keratitis. In: Holland EJ, Mannis MJ, Lee WB, editors. Ocular Surface Disease: Cornea, Conjunctiva, and Tear Film. Philadelphia: Elsevier Saunders; 2013. P. 213-16.
Zaidman GW, Geeraets R, Paylor RR, et al. The histopathology of filamentary keratitis. Arch Ophthalmology 1985; 103: 1178-81.
Tanioka H, Yokoi N, Komuro A, et al. Investigation of the corneal filament in filamentary keratitis. Invest Ophthalmol Vis Sci 2009; 50:3696-702.