Corneal Tattoo or Keratopigmentation:
How to Help Eye Look Normal and/or Help Glare Symptoms
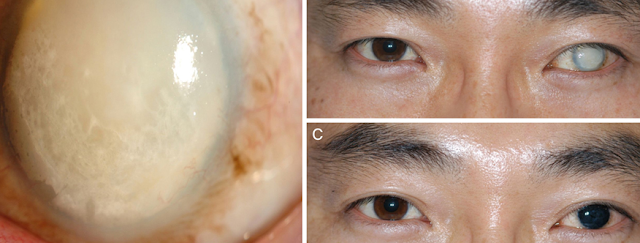
Some patients who loose vision in the eye or have a metabolic abnormality can develop a white or opacified cornea.
This can be cosmetically unacceptable.
For this we use Corneal Tattoo or Keratopigmentation with or without a Femtosecond Laser.
In some patients who have a laser applied to the eye (either RK [Radial Keratometry], LASIK, PRK, or Laser Iridotomy for narrow angle) or after a corneal transplant [PK: penetrating keratectomy], symptoms of severe glare can become an issue. It is very rare with most lasers but can happen.
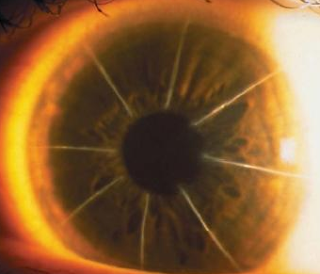
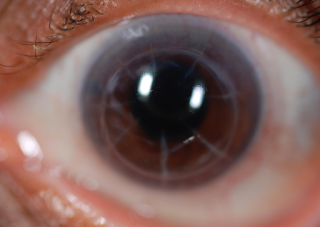
Below is an example of an patient who had glare after a laser peripheral iridotomy for narrow angle (which is a potentially blinding disease process) done in England. A corneal tattoo was performed to help with these glare complaints.
Glare after a laser iridotomy is very rare but can happen.
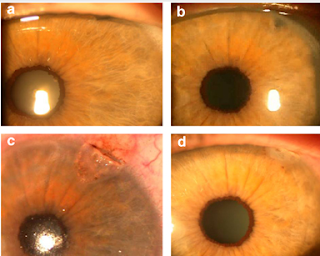
Corneal Tattoo or Keratopigmentation is an excellent option to help patients improve their cosmetic appearance if their cornea are white and opacified or if a patient is having significant glare from a laser procedure.
We perform Corneal Tattoo or Keratopigmentation at our office and also use a Femtosecond laser as noted below by my friend, Dr. Pineda at Harvard’s Massachusetts Eye and Ear Infirmary.
Roberto Pineda, MD, Boston, presented on FLAK.
Keratopigmentation has been around for some time, he said. It is a form of anterior segment reconstruction using a corneal tattooing treatment. It’s been used for centuries, traditionally for cosmetic purposes, but now is being used for optical function. However, he noted that this procedure is not like the dangerous conjunctival tattooing that has become popular in some places.
Keratopigmentation (KTP) is now done with micronized mineral pigments and new surgical techniques, Dr. Pineda said. It’s possible to manage moderate to severe visual dysfunctions related to iris defects. KTP is minimally invasive, he said, and new study results found a decrease in subjective glare, photophobia, and monocular diplopia.
Indications for keratopigmentation include symptomatic peripheral iridectomy, traumatic aniridia, traumatic coloboma, atrophic and fixed dilated iris, and iridocorneal endothelial syndrome. It also has cosmetic indications in a low visual potential cornea.
In traditional KTP, the physician denudes the corneal epithelium with a blade or excimer laser, Dr. Pineda said. Use a 27- or 30-gauge needle at an oblique angle for application of the pigment into the corneal stroma, he said.
Dr. Pineda then described his technique for FLAK, which includes using topical anesthesia, 2 separate corneal pockets, a circular center pocket to simulate the pupil, and a peripheral channel to simulate the iris.
“With this technique, you can customize the dimensions of the treated area,” he said. There are well-defined lamellar dissections; it’s faster than conventional treatments, less painful, and theoretically less likely to fade, he added.
“Obviously, there are some limitations,” Dr. Pineda said. “It does require a relatively clear cornea.” There are also limited tattoo pigment colors, and extensive keratopigmentation can limit visualization of intraocular structures if they require monitoring, he said.
Potential complications to be aware of with keratopigmentation include under pigmentation, over pigmentation, pigment migration, infection, perforation, delayed healing, and uveitis.
Dr. Pineda said there are still factors to investigate for the future. “We want to continue to monitor the long-term effects of these dyes,” he said. The need for tattoo enhancement in the future may also warrant further investigation. He thinks FLAK is an effective technique and is an alternative method of keratopigmentation for the treatment of problematic PIs, corneal leucomas, or leukocoria, despite its added expense.
References:
The Epidemiology of Cosmetic Treatments for Corneal Opacities in a Korean Population
Ki Cheol Chang,1,2 Ji-Won Kwon, 1,3 Young Keun Han,1,4 Won Ryang Wee,1 and Jin Hak Lee1,5
1,3 Young Keun Han,1,4 Won Ryang Wee,1 and Jin Hak Lee1,5
1Seoul Artificial Eye Center
The Korean Ophthalmological Society