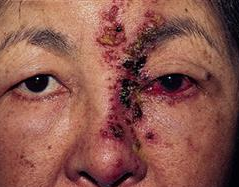
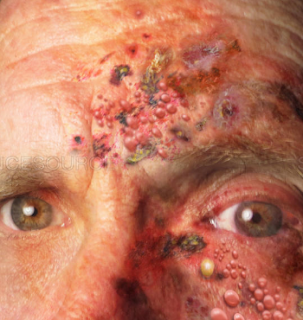
I remember when we used to do a full autoimmune workup for every Shingles patients younger than 50. We used to all be worried there was an underlying immune issue.
We now know that the rates of Shingles in patients under 60 have been increasing and the age of presentation is also decreasing.
Shingles can cause debilitating pain if not treated urgently. The risk of Postherpetic neuralgia, particularly in patients over 70years old is high. PHN is continued pain beyond 3 months after the onset of tShinglesges. It is the most common and devastating complication of Shingles. PNH occurs in about 30% of patients and is the most common cause for suicide in 70+-year-olds.
Another friend had Shingles when he was 49. He went to the best doctors in his town of Boston, but for some reason that I just cannot understand, they did not give him PHN prevention medication. He now lives with PHN which has been at times a real issue.
There are 2 key vaccines to prevent the recurrence of Shingles.
Note Herpes Zoster and Herpes Simplex are 2 completely different viruses and have different presentations. There are no vaccines against Herpes Simplex which has 2 types: HSV 1 which is the common cold sore and HSV 2 which is gential herpes and debilitating.
For Herpes Zoster or Shingles:
1. Zostavax: this is the 1st vaccine developed
-AAO recommends getting this vaccine in all patients 50 or older
-this is a live attenuated virus
-patients taking antiviral pills need to stop the pills 1day before vaccination and stopped for 2wks after vaccination, and then resume the pills
-there have been cases of reactivation of HZ keratitis reported within 2-5wks after this vaccine.
-if a patient has a history of HZ keratitis, they need to be told of this risk & to return if new symptoms develop and/or followed 4-6 wks after vaccination
2. Shingrix: FDA approved 2017
-not a live virus
-for patients 50yrs or older
-97% effective for age groups 50-69 and 91% effective for patients 70 & older
-those who have received Zostavax need to be revaccinated with Shingrix.
-involves 2 intramuscular injections 2-6 months apart
-more cost-effective compared to Zostavax.
Treatment of HZV:
1. High dose antiviral: Valcyclovir 100mg tid po within 72 hrs of onset of rash.
Slow taper to below
2. Treat corneal issue with steroids if stromal.
Prevention of Reactivation:
For Herpes Simplex:
The Herpetic Eye Disease Study showed Acyclovir 400mg po bid helps decrease risk of recurrence 45%.
For Herpes Zoster:
Valcyclovir 500mg qd or Acyclovir 500mg po bid reduces recurrence 35%.