Lipiflow May Help Symptoms of Blepharochalasis
Blepharochalasis is a not too common condition thought to be a familial variant of angioneurotic edema (ie, swelling under the skin: more info below at end of blog post **). The exact cause is not known. It tends to occur in younger women (compared to Dermatochalasis–sounds the same but in older patients with lax upper eyelid skin that can sag).
Signs of Blepharochalasis:
-cigarette paper skin (eg, wrinkly skin)
-relapsing and remitting edema (eg, swelling comes & goest)
-subcutaneous telangiectasia (eg, fine red lines under skin)
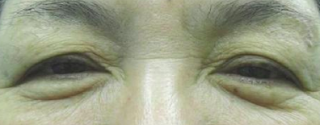
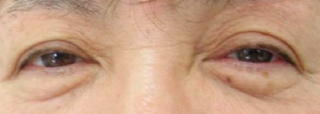
This is a patient before eyelid surgery called blepharoplasty for the Blepharochalasis
There are few treatment options Blepharochalasis. If it is due to an allergy or anything in the below Differential Diagnosis, it can be easier to remedy. Blepharochalasis is more of a diagnosis of exclusion: if you exclude most of the below, it is likely Blepharochalasis.
Differential diagnosis (eg, what to think about and consider ruling out):
1. Dermatochalasis: lax or redundant upper eyelid skin commonly associated with aging
2. Thyroid eye disease:
3. Floppy eyelid syndrome:
4. Orbital cellulitis:
5. Sarcoidosis:
6. Idiopathic orbital inflammation:
7. Hereditary angioedema:
8. Dacryoadenitis:
9. Lacrimal gland tumor:
10. Localized cutis laxa:
11. Hormonal changes especially during puberty:
12. Upper respiratory tract infections:
13. Allergies may also play a role in Blepharochalasis:
What can maybe make Blepharochalasis worse potentially:
1. Aging
2. Hormonal changes
3. Stress
4. Allergies
5. Diet
Treatment:
There is no established treatment protocol for blepharochalasis.
Studies have shown the below do not help:
-Systemic or topical steroids,
-Antihistamines and other anti-inflammatory agents
Experimental treatments have been reported in the literature:
1. Oral doxycycline (inhibitor of matrix metalloproteinases):
a. 2 patients reported to improve eyelid edema and prevent recurrent attacks: 50 mg po bid initially, then tapered to 25 mg po qod
b. there are no trials to evaluate the safety and efficacy of long term use of doxycycline in blepharochalasis syndrome.
2. Oral sustained release acetazolamide:
a. 250 mg po qd reduced periorbital edema and lid discomfort in a patient who refused surgery and failed treatment with oral
b. side effects caused drug acetazolamide to be discontinued after a short course.
3. Surgery may help, but may not be a cure. The difference in the above photos was minimal but the patient may have been very happy.
***4. Lipiflow or Thermal Pulsation: I have had 2 patients who feel Lipiflow helped their Blepharochalasis. This has not been reported as of yet. If we get another couple of patients who report this, we will publish this observation. Lipiflow is very low risk. NO surgery required. NO steroids required. There have been no studies to evaluate meibography with symptoms of Blepharochalasis. It could be there is a relationship and Lipiflow milks out clogged oil which can lead to less swelling. Or Lipiflow decreases inflammation within the lid or ocular surface, which then leads to improvement. A prospective, double blind study would need to be done but that will take years as it is hard to do thermal pulsation/Lipiflow only on 1 eye’s eyelids.
References:
1. Infraeyebrow Blepharoplasty for Blepharochalasis of the Upper Eyelid: Its Indication and Priority
Abstract
Eyelid bags and blepharochalasis are the result of relaxation of lid structures like the skin, the orbicularis oculi, and mainly the orbital septum. Therefore, this aged appearance cannot be improved sufficiently with only a skin and orbicularis oculi resection. To improve this appearance, we use a very effective method of tucking of the orbital septum with infraeyebrow excision of the skin and the orbicularis oculi. Between January 2005 and April 2011, 103 patients (206 lids) were treated. There were 89 female and 14 male patients whose ages ranged from 43 to 75 years (mean = 65.2 years). After infraeyebrow excision, blepharoplasty with tucking of the orbital septum, the concealed lid crease becomes apparent and a good rejuvenation effect is obtained in all patients.
2.
https://eyewiki.aao.org/Blepharochalasis_Syndrome
Disease Entity
Blepharochalasis or blepharochalasis syndrome is a rare condition characterized by episodic inflammation of the eyelids.
Disease
This condition was initially described by Beer in 1817, but the term blepharochalasis was assigned to this entity by Fuchs in 1896. [1] This disorder typically affects the upper eyelids and usually occurs bilaterally, though rare cases of unilateral presentations and lower eyelid involvement have been reported.
Stages of blepharochasis syndrome including an active intumescent phase during which attacks of non-pitting edema will occur, and a subsequent atrophic, quiescent phase characterized by the absence of attacks for two years and paper-thin, baggy eyelid skin, have been described. [1] [2] Attacks often last two to three days but this is highly variable between patients. The frequency of edema attacks is usually in the range of three to four episodes per year early in the disease course. [2]
Etiology
Unlike dermatochalasis which may often be confused with this disorder and is an involutional change of the eyelid, blepharochalasis is thought to be a familial variant of angioneurotic edema. While the exact underlying cause is not known, there have been multiple systemic associations described. A link to Asher’s syndrome, a rare condition characterized by attacks of upper eyelid and lip edema with or without euthyroid goiter, has been suggested.[1] Other theories suggest hormonal changes especially during puberty, upper respiratory tract infections, and allergies may also play a role in the disease process.
Epidemiology
Because it is a rare syndrome, minimal epidemiologic data is available. Blepharochalasis has been reported more in females, though it is thought that it affects both genders at similar rates. Patients report more frequent attacks during adolescence or young adulthood followed by less frequent attacks during adulthood.
General Pathology
The underlying pathology has not been studied extensively for this disease process. However, several case reports have demonstrated distinct findings in the affected eyelid tissues at the cellular level supporting an underlying immunopathogenic process. Eyelid biopsy in a single patient with blepharochalasis revealed perivascular and interstitial infiltration of lymphocytes in the dermis associated with a marked decrease in elastic fibers. Staining of MMP-3 and MMP-9 was detected in and around infiltrating cells in the dermis. [3] In another study, abundant IgA deposits surrounding atrophic elastic fibers in the eyelid skin of a patient was reported, while these deposits were absent in a control sample of a remote skin biopsy site. [4]
Pathophysiology
Several theories regarding the pathogenesis and pathophysiology of blepharochalasis have been explored, though none has been confirmed. The episodic eyelid edema which regresses spontaneously may be suggestive of idiopathic angioedema, wherein extravasation of fluid from capillaries causes localized edema. The result is stretched, atrophic tissue. However, perivascular infiltrates which have been reported on histologic examination of eyelid tissue in patients with blepharochalasis may support an alternative or concomitant inflammatory process. [2] Why this inflammation or idiopathic angioedema is confined to the eyelids also remains unknown.
Diagnosis
History
Patients will frequently describe attacks of painless eyelid swelling, sometimes associated with erythema. In most cases, triggers are not identified. Some may report stressful events preceding attacks of edema, or a history of allergy. [1] Other reported triggering factors include crying, bee sting, fever, wind and physical activity. [2]
Physical examination
Blepharochalasis is a clinical diagnosis. In the acute phase, characteristic findings eyelid edema, erythema, and conjunctival injection. A wide variety of physical exam findings may be present and include:[1]
- “Cigarette paper” or finely wrinkled skin
- Severe eyelid skin thinning
- Lax eyelid skin which may obstruct vision
- Entropion and ectropion
- Subcutaneous telangectasia
- Pigmentary skin changes
- Levator dehiscence ptosis
- Orbital fat prolapse
- Lacrimal gland prolapse
- Pseudoepicanthal fold with atrophy of the nasal fat pad
- Proptosis
Laboratory test
Laboratory studies do not currently play a role in the diagnosis of blepharochalasis syndrome.
Differential diagnosis
Dermatochalasis, which refers to lax or redundant upper eyelid skin commonly associated with aging, may be confused with blepharochalasis. However, dermatochalasis is not associated with the characteristic findings of blepharochalasis, namely cigarette paper skin, relapsing and remitting edema, and subcutaneous telangiectasia. [1] Patients with dermatochalasis will also tend to be older than those affected by blepharochalasis.
Other diagnoses to consider would include thyroid eye disease, floppy eyelid syndrome, orbital cellulitis, sarcoidosis, idiopathic orbital inflammation, hereditary angioedema, dacryoadenitis, lacrimal gland tumor, and localized cutis laxa.[1]
Management
Medical therapy
There is no established treatment protocol for blepharochalasis. Systemic or topical steroids, antihistamines and other anti-inflammatory agents have not been shown to play a role in acute attacks or in the overall disease course.
Experimental treatments have been reported in the literature. Oral doxycycline, a known inhibitor of matrix metalloproteinases, has been described in a case report of two patients to improve eyelid edema and prevent recurrent attacks. The patients were treated with a dose of 50 mg po bid initially, then tapered to 25 mg po qod. [5] However, there have been no trials to evaluate the safety and efficacy of long term use of doxycycline in blepharochalasis syndrome.
In another case report, oral sustained release acetazolamide at a dose of 250 mg po qd reduced periorbital edema and lid discomfort in a patient who refused surgery and failed treatment with oral corticosteroids. [6] Given the side effect profile of acetazolamide, the drug was discontinued after a short course.
Surgery
Surgical interventions are aimed at correcting the complications of blepharochalasis, most commonly ptosis and eyelid skin laxity. Surgical correction should be delayed until late in the disease course when attacks have become infrequent. Disease quiescence for six to twelve months is recommended prior to surgery. [1] [2]
Blepharoplasty, levator aponeurosis dehiscence repair, eyelid tightening, canthal tendon reattachment, and fat grafting may all be considered for these patients.
Unfortunately, the same inflammatory process which results in the blepharochalasis may cause ptosis and eyelid skin laxity to recur after surgical repair. [7] Patients should, therefore, be counseled appropriately.
Complications
Ptosis, herniation of the orbital lobe of the lacrimal gland, prominent eyelid vascularity, and orbital fat pad atrophy are all complications which may arise from this condition. [7]
Prognosis
There is insufficient data regarding changes in the frequency of attacks prior to and following surgery. Treatments in the future will likely be aimed at preventing the condition and the complications associated with this disorder ultimately to avoiding the need for surgical correction of these sequelae.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Kotlus B. Blepharochalasis syndrome. http://emedicine.medscape.com/article/1214014-overview#a9. Mar 23, 2015.
- ↑ 2.0 2.1 2.2 2.3 2.4 Koursh DM et al. The blepharochalasis syndrome. Surv Ophthalmol. 2009 Mar-Apr;54(2):235-44.
- ↑ Motegi S et al. Blepharochalasis: possibly associated with matrix metalloproteinases. J Dermatol. 2014 Jun;41(6):536-8.
- ↑ Grasseger A et al. Immunoglobulin A (IgA) deposits in lesional skin of a patient with blepharochalasis. Br J Dermatol. 1996 Nov;135(5):791-5.
- ↑ Karaconji T et al. Doxycycline for treatment of blepharochalasis via inhibition of matrix metalloproteinases. Ophthal Plast Reconstr Surg. 2012 May-Jun;28(3):e76-8.
- ↑ Lazaridou MN, Sanding T and Kemp EG. Oral acetazolamide: A treatment option for blepharochalasis? Clin Ophthalmol. 2007 Sep; 1(3): 331–333.
- ↑ 7.0 7.1 Basic Clinical Science Series. Orbit, Eyelids, and Lacrimal System. American Academy of Ophthalmology. 2014-2015
Angioedema is swelling beneath your skin which can for large, thick, firm welts with redness, warmth, and pain. It can happen at many points on your body, including your:
- Face
- Throat: if happens seek medical help asap
- Larynx (your voice box): if happens seek medical help asap
- Uvula (the little piece of skin that hangs from the back of your throat)
- Arms
- Hands
- Legs or feet
- Genitals: sometimes with hives
- Intestine
Types and Causes
There are 4 types of angioedema:
1. Allergic angioedema: *Most common. Allergy can be due to:
- Shellfish
- Fish
- Peanuts
- Tree nuts
- Eggs
- Milk
- Pollen
- Animal dander
- Latex
- Insect stings
2. Drug-induced angioedema: Some medicines trigger angioedema.
- Penicillin
- Aspirin
- Other non-steroidal anti-inflammatory drugs (NSAIDs), like ibuprofen.
- Blood pressure medicines called angiotensin-converting enzyme (ACE) inhibitors ; sudden reactions after years of use have been reported
3. Hereditary angioedema (HAE): This is rare. It happens when your body doesn’t make enough of a blood protein called C1 esterase inhibitor. That lets fluid from your blood move into other tissues, which brings swelling.
You’ll usually have your first bout of this before you turn 12 years old. You may pass the condition on to your children.
There’s another very rare type called acquired angioedema that has the same symptoms as HAE. It’s different because it doesn’t happen until you’re older than 40. It usually happens when you have a weakened immune system. Unlike HAE, you can’t pass it on to your children.
4. Idiopathic angioedema: Idiopathic means there isn’t a known cause for your swelling. Possible culprits can include:
- Anxiety or stress
- Minor infections
- High or low temperatures
- Overdoing it when you exercise
Allergic and drug-induced angioedema usually happen within an hour of exposure to your trigger. Hereditary and acquired types usually happen over many hours, but it can feel much faster if you wake up and suddenly discover swelling.
Who Gets It?
You may have a higher chance of angioedema if:
- You’ve had hives, allergic reactions, or if you’ve had angioedema before
- You have lupus, lymphoma, thyroid disease, hepatitis, HIV, cytomegalovirus, Epstein-Barr virus, or have had a blood transfusion
- You have a family history of hives or angioedema
- You have asthma and take NSAIDs
- You take ACE inhibitors. This is especially true if you’re a woman or African-American, or if you take angiotensin receptor blockers (ARBs).
- You’ve had recombinant tissue plasminogen activator (rtPA ) therapy for a stroke
Diagnosis
To find out what type of angioedema you have, your doctor will examine you and talk about your symptoms. They may do blood tests to get more details.
Treatment
Angioedema usually gets better on its own within a few days. If you do need treatment, it can include:
- Medicines to ease swelling and inflammation, like antihistamines and oral corticosteroids
- Drugs to slow down your immune system if antihistamines and corticosteroids don’t work
- Other medicines that ease pain and swelling, like leukotriene antagonists (a group of anti-inflammatory medicines that aren’t steroids)
- Blood protein controllers if you have hereditary angioedema
If your angioedema is drug-induced, your doctor will usually switch you to another medicine that you can handle better.
For a serious attack, you may need a shot of epinephrine (a type of adrenaline). For repeated strong attacks, you may need to carry a pen-like device so you can inject yourself with epinephrine in an emergency.
Prevention
You can avoid allergic episodes if you stay away from foods, medications, or other conditions that trigger angioedema. If you don’t know what’s causing your episodes, try to keep a diary to track of foods, symptoms, and situations tied to your symptoms.
Your doctor might suggest you take antihistamines every day instead of just when you need them. This can help get rid of episodes, make them happen less often, or be less dangerous. You also won’t have to wait for the medicine to start working when you need relief.