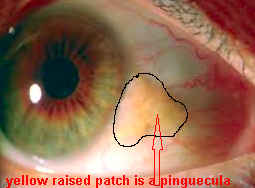
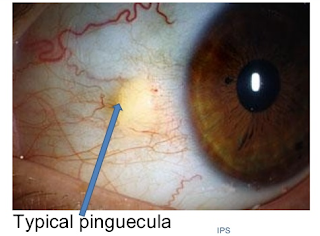
Yellow Eyes: Is it Jaundice or Prominent Pingueculas or Pterygia
A Patient from India asked:
I have yellow eyes what should I do?
Answer:
Please send us photo first. It could be jaundice or very noticeable pingueculas or pterygium: the work up for each is very different. If Jaundice, you need to have liver function tests, check for hepatitis & urine test for bilirubin, which indicates that conjugated hyperbilirubinemia is present.
Explanation:
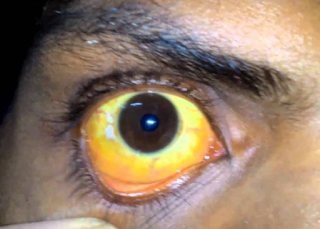
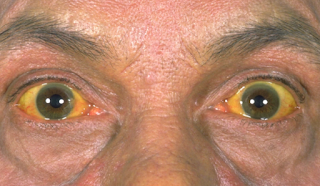
These patients have true jaundice with yellow sclera (the white wall of the eyeball).
The word “jaundice” comes from the French word jaune, which means yellow. Jaundice is a yellowish staining of the skin, sclera, and mucous membranes by bilirubin, a yellow-orange bile pigment. Bilirubin is formed by a breakdown product of heme rings, usually from metabolized red blood cells. The discoloration typically is detected clinically once the serum bilirubin level rises above 3 mg per dL (51.3 μper L).
Jaundice is not a common presenting complaint in adults. When present, it may indicate a serious problem.
The classic definition of jaundice is a serum bilirubin level greater than 2.5 to 3 mg per dL (42.8 to 51.3 μper L) in conjunction with a clinical picture of yellow skin and sclera. Bilirubin metabolism takes place in three phases—prehepatic, intrahepatic, and posthepatic, thus we usually classify jaundice as to where the defect is. See below for more details.
Sandra Lora Cremers, MD, FACS
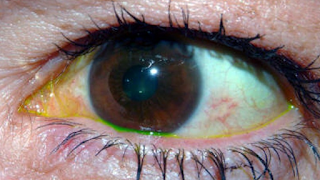
These patients below have yellowing of the growth on the conjunctiva (the usually clear covering of the white part of the eye called the sclera).
The last photo above has a pinguecula near the nose on the left & near the temple area on the right but fluorescein drops were placed so a thin layer of yellow is seen along the lid margin.
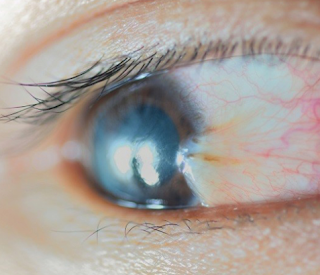
This patient below has a pterygium which can sometimes have a yellow tinge to it. A pterygium is an abnormal growth onto the surface of the eye (cornea: the window of the eye) coming from the conjunctiva (the usually clear tissue covering the white part of the eye).
The Differential Diagnosis of Jaundice is best classified by location: Hepatic means liver.
1. prehepatic
2. intrahepatic
3. posthepatic
Details
1. Prehepatic causes of jaundice include:
a. hemolysis and hematoma resorption, which lead to elevated levels of unconjugated (indirect) bilirubin.
2. Intrahepatic disorders can lead to unconjugated or conjugated hyperbilirubinemia. The conjugated (direct) bilirubin level is often elevated by
a. alcohol,
b. infectious hepatitis,
c. drug reactions, and
d. autoimmune disorders.
3. Posthepatic disorders also can cause conjugated hyperbilirubinemia.
a. Gallstone formation is the most common and benign posthepatic process that causes jaundice; b. biliary tract infection,
c.pancreatitis,
d. malignancies.
Work Up:
1. urine test for bilirubin, which indicates that conjugated hyperbilirubinemia is present.
2. complete blood count
3. Liver function tests
4. Hepatitis A, B, C titiers
If all negative, get:
6. abdominal imaging by ultrasonography or computed tomographic scanning.
Rarely may need:
7. more invasive procedures such as cholangiography or
8. liver biopsy may be needed to arrive at a diagnosis.