Docetaxel Destroys Meibomian Glands in Some Patients
I am suspicious that Docetaxel Destroys Meibomian Glands in Some Patients. I cannot prove this yet and have only 2 patients who have been on Docetaxel with terrible dry eye disease. There are no papers to state this either.
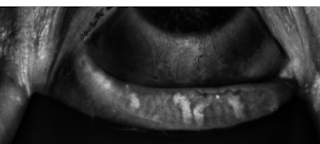
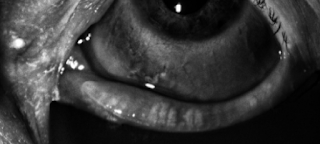
But above you can see the loss of Meibomian glands in a patient who has been on a couple of cycles of Docetaxel for breast cancer: (the white lines are the glands: there should be about 25-30 of them. All that is left are a few glands on the upper photo; more on the bottom photo).
If you have ever had Docetaxel and have dry eyes, let me know. If you are about to start Docetaxel, please let us take a Lipiscan of your meibomian glands before and after treatment to see if this affects your glands.
Here is some research on the topic.
Sandra Lora Cremers, MD, FACS
Docetaxel-induced Meibomian duct inflammation and blockage leading to chalazion formation.
https://www.nature.com/pcan/journal/v10/n4/pdf/4500939a.pdf?origin=publication_detail
[The pathology of ocular syndromes caused by toxicity].
[Article in French]
Abstract
Ocular adnexa represent a complex system of delicate organs and functions which are the target of varied side effects. Most involve more than one component at a time, however landmark signs and symptoms can be outlined. Dry eye leads the list. The aqueous production of the tear film can be decreased by certain psychotherapeutic agents (especially the older ones), while the phospholipidic component, produced by the Meibomian glands, can be markedly affected by retinoids. On the other hand, cytostatic drugs like Docetaxel (and 5-FU at a lesser degree) frequently induce canalicular stenosis, resulting in epiphora. Amongst a long list of substances, diphosphonates used in the treatment of osteoporosis and phosphodiesterase-5 inhibitors used in erection deficiencies induce conjunctival irritation, either directly or by contiguity. Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis represent the most severe toxic insult to the mucosae. A recent chemotherapeutic agent, Imatinib, induces fluctuant palpebral edema in a majority of patients. Despite being applied topically, prostaglandin analogs exert a profound effect onto the cellular physiology of the eyelash and the ocular and palpebral melanocyte. Indirectly, immunosuppressive agents used in graft rejection control have been associated with the emergence of secondary neoplasia, mainly lymphoma, of which the orbit is a rare but possible location. Chronic administration of steroid drugs leads to hypertrophy of the orbital fat and proptosis.